Most women wait years for answers. Bloom gives you a detailed clinical picture of your own anatomy so you can stop guessing and start knowing.
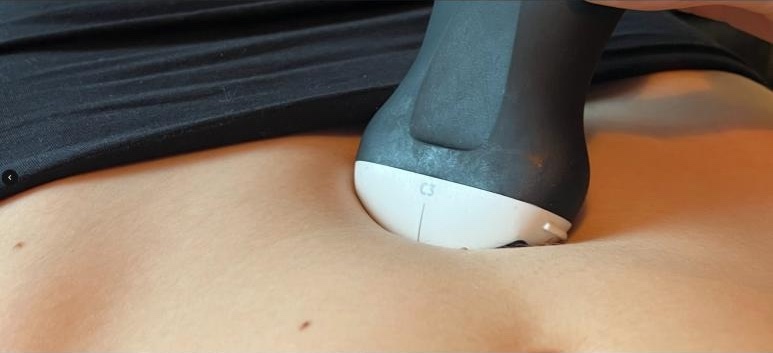
Bloom gives you daily clinician-reviewed imaging to bring to any specialist; concrete documentation that can compress years of uncertainty into weeks.